So much to report! This is going to be fact / text heavy but I want to make sure I get thru all the details.
On Thursday, I met with Dr. Sink at HSS (full disclosure, I asked – he was cool using his last name on the blog) for my 6 week follow-up, although it had been exactly 7 weeks since my surgery. I took a cab to the appointment since I was not yet comfortable with the idea of taking the subway (and would have been exhausted since HSS is about the length of 7 avenue blocks from the subway).
When I first got there, I had 2 x-rays taken and was immediately whisked into an exam room. Dr. S’s nurse and PA came in to talk to me initially, to see how I was feeling and how recovery had been going. I was in a really good mood — in fact, I’ve been in a really good mood for most of my recovery (which likely has more to do with not being as hyper-stressed [from trying to juggle school / work / social life] than with recovering from an invasive operation). In any event, we had a good chat and they seemed pleased with how I was doing.
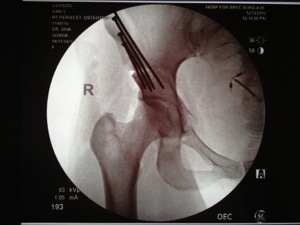
Dr. S. came in a few minutes later and we started talking about how my healing was going. I told him that I felt really good, that I was using the crutches when I went short distances and a wheelchair for long distances (walker when at home). He looked at the x-rays and confirmed that 1) the bone was filling in really nicely along all of the breaks, 2) that the head of my right femur is now sufficiently covered by my right acetabulum, and 3) that the angles (between the center of the head of the femur / hip) created the perfect 90% angle that he was looking for. He seemed really psyched about that and I was pleased to know that the surgery appears to have turned out really well. He also confirmed that I have 5 screws (I had only noted 4) and that I was ready to move onto physical therapy 1/2 x week x 8 weeks. More on that later.
We then started talking about my left hip, what type of surgery we would be looking at, especially since the surgery is scheduled for May 8th. As a reminder, although my right hip had dysplasia (which can only really be solved by a PAO), my left hip has acetabular retroversion, mild femoral retroversion, cam and pincer impingement, the neck of my femur (between the ball and trochanter) is too short, multiple labral tears, a hairline fracture of the acetabulum and what appears to be a hypertrophic (overdeveloped) labrum. We had always discussed an SDD for the left hip but at my last few appointments, Dr. S suggested that the left hip might need a reverse PAO so I was curious what he would say, having now reconfigured my right hip. After some discussion about the coverage of my femur (which looks good, side to side), he feels that an SDD is the best way to go. What this will mean is that the incision will be on the rear side of my left thigh, 8″-10″ long, and during the procedure Dr. S. will literally remove my femur from the socket, shave down the impingements on the femur and acetabulum, repair the labrum, break the trochanter and either move or remove a part of it, remove and reattach muscles, and I don’t know what else, but not necessarily in that order. As much of an invasive procedure the PAO was, this actually sounds worse. But strangely, I am totally not concerned.
The plan is that I will meet him in 6 weeks, after my PT, to see how I’m doing. Things may change and the surgical plan is fluid but at this point, an SDD is the plan. Dr. S was great, explaining all of the reasonings for doing this procedure and showing me the x-rays and MRI scans. I was at his office for about and hour and fifteen minutes and he was in the room talking to me and my husband for the majority of the time.
After my appointment I met with a physical therapist who gave me some initial exercises to perform at home. I was shocked to be told I could be full weight bearing on my crutches (and am permitted to use only 1 crutch or a cane when at home). Some of my exercises require that I stand on only one leg – the operated leg – and I was really surprised that I was able to do all of it with no pain (although my muscles are way weak). I’ll start PT in Brooklyn next week.
Finally and un-hip related, I went and had a CT scan of my sinuses / maxillofacial bones to see if there is any reason I am permanently congested / have terrible allergies in spite of allergy shots + major pills. My ENT thinks it might have more to do with the fact that I have a very small nose and that the sinuses are so small that there’s simply no space to move around. There has been suggestion of sinus surgery to see if there is some space to be opened up. I seriously need a break from surgery, not more! We’ll see what shows up those reports.
I feel like you seriously deserve a prize if you got all the way to this point in the post. I hope my honest to goodness gratitude is prize enough, but seriously, thanks so much for reading. Onward and upward (or, actually, downward since I need to do my PT exercises before bed). G’night!